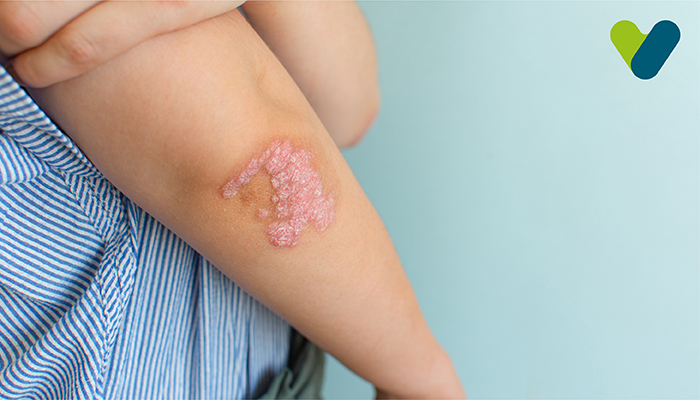
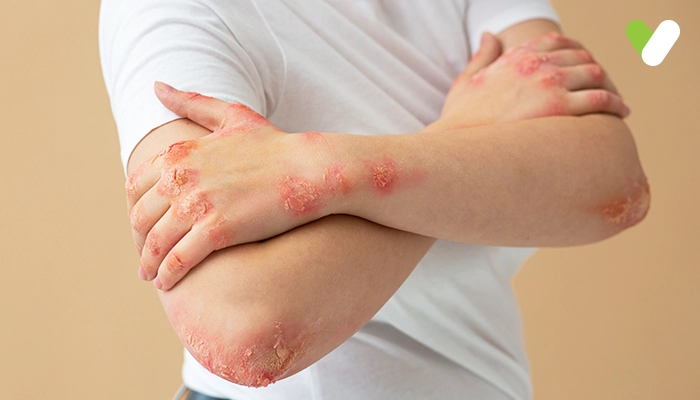
Psoriasis is a rash or a chronic autoimmune skin condition that causes skin build-up into rough red patches covered with white scales. It is a skin disorder where the skin cells multiply faster than usual, growing deep in your skin and slowly rising to the surface to fall off eventually. Psoriasis symptoms usually appear on the scalp, elbows, knees, and lower back. However, they can develop in other areas of your body, like the hands, feet, neck, scalp, and face. Psoriasis can occur in members of the same family.
Psoriasis is associated with several other conditions like the following: • Type 2 diabetes • Inflammatory bowel disease • Heart disease • Psoriatic arthritis • Anxiety • Depression
Psoriasis is not contagious
One cannot infect a person with a skin condition. Touching a psoriatic lesion will not infect you and cause you to develop the condition. Psoriasis is not contagious.Symptoms of Psoriasis
PlaPsoriasis symptoms or flare-ups differ from person to person. Symptoms also depend on the type of psoriasis. Not everybody will experience all these symptoms enlisted below.Common symptoms of plaque psoriasis include the following: • Inflamed red skin patches on lighter skin and brown or purple on darker skin • Dry skin that cracks or bleeds • Soreness around patches • Itching and burning sensations around patches • Thick, pitted nails • Painful, swollen joints
Most people with psoriasis go through symptom cycles. Patients experience severe symptoms for some time, after which the symptoms become almost unnoticeable before flaring up again. Sometimes, psoriasis symptoms disappear entirely. You may be in remission when you have no active signs of the condition, but you are still at risk of a relapse.
Causes of Psoriasis
The cause of psoriasis still needs to be fully understood. Many studies have not yet established psoriasis causes, although research indicates that there are two key factors:(a) Genetics: Some patients inherit the genes or the conditions that make them more likely to develop psoriasis. Schedule a dermatologist consultation if you observe some skin discomfort and have an immediate family member with the skin condition, as you may also manifest the disease in your lifetime.
(b) Immune system: Psoriasis is an autoimmune condition. What does this imply? Generally, in the body, white blood cells attack and destroy the invading bacteria and mount a defence against infection. Thus, the autoimmune attack on the body's skin triggers sped-up skin cell production and skin cells develop too quickly, which rise to the skin's surface, where they pile up. The attacks on the skin cells also lead to inflamed skin that becomes red.
Diagnosis of Psoriasis
Set aside time for a dermatologist consultation to diagnose psoriasis if you have a rash on your scalp, ears, elbows, knees or nails. Also, let your specialist know if family members have the condition.• Lab tests: You may undergo a basic full-body checkup and a skin biopsy. The biopsy entails extracting and testing a skin patch and is carried out at your specialist's office. The technicians will send the skin biopsy sample to a lab for analysis to determine psoriasis and rule out other infections. Your skin specialist will then discuss the findings and current treatment options
Types of Psoriasis
There are about five general types of psoriasis, each of which has a set of symptoms:• Plaque psoriasis: The most common type, it causes dry, itchy, raised skin patches covered with scales. The inflammations usually appear on the arms, elbows, knees, lower back and scalp areas. The patches vary in colour, depending on skin colour.
• Nail psoriasis: Psoriasis can also affect your fingernails and toenails, causing pitting, abnormal nail growth, and discolouration. Affected nails might loosen from the nail bed, which is called onycholysis. At a severe stage of the disease, the nail eventually loosens from the nailbed and crumbles.
• Guttate psoriasis: This type of psoriasis primarily affects young adults and children. Bacterial infections such as strep throat, tonsillitis, skin injury, or antimalarial and beta-blocker medications can trigger Guttate psoriasis. Its symptoms appear like small, drop-shaped scaling spots on the trunk, arms or legs.
• Inverse psoriasis: It primarily affects the skin folds around the groin, buttocks and breasts. Inverse psoriasis triggers smooth patches on inflamed skin that worsen with friction and sweating and cause discomfort.
• Pustular psoriasis: The type of psoriasis, a less common and leads to pus-filled blisters. Pustular psoriasis occurs in widespread patches on the body or smaller areas of the palms or soles of feet.
• Erythrodermic psoriasis: It is a rare type of psoriasis that can appear across the entire body as a peeling rash that can cause itching or burn intensely. It can be both short-lived (acute) or long-term (chronic).
When to consult a specialist?
If a family member already has psoriasis, remember to undergo a basic full-body checkup and regularly do the same for your children. If you suspect that you have the condition, book an appointment for a dermatologist consultation if your condition: • Becomes severe or widespread • Causes you discomfort, itching and painPsoriasis can be mistaken for Eczema
Although the symptoms of both conditions are similar, psoriasis and eczema are two unrelated skin conditions. Both conditions have similar symptoms like discoloured skin, a rash and itching. Psoriasis plaques cause areas of thick skin covered in scales. In contrast, eczema causes inflammation of dry and bumpy skin. Also, eczema typically causes more intense itching than psoriasis.Psoriasis Triggers
Many people predisposed to psoriasis may be symptom-free for years until some environmental factor triggers the condition.The most common psoriasis triggers include:
• Stress: Stress is one of the most common psoriasis triggers. At the same time, a psoriasis flare-up can also cause anxiety, making it seem like an endless loop. However, relaxation techniques and stress management can help elevate stress from impacting psoriasis.
• Skin injury: Psoriasis can manifest in areas of the skin that have been injured or affected, like scratches, sunburns, bug bites and vaccinations.
• Illness: Anything infection that affects the immune system can trigger psoriasis. Many patients experience an outbreak following an ear infection, bronchitis, tonsillitis or respiratory infection. For instance, there is a connection between streptococcus infection and guttate psoriasis. Strep throat often triggers the onset of guttate psoriasis in children. Strep throat is a bacterial infection that leads to a sore and scratchy throat. Also, you can have strep throat without any symptoms. Thus, if you have had strep throat in the past, discuss your medical history with your skin specialist.
• Weather: Certain weather conditions can trigger an outbreak. For instance, cold weather can cause psoriasis flares due to less sunlight and humidity and heated and drier indoor air. On the other hand, warm weather can reduce psoriasis symptoms because of natural sunlight and higher humidity levels.
• Alcohol: An alcohol disorder can trigger psoriasis flare-ups. If you over-consume alcohol, psoriasis outbreaks may be more frequent. Reduce alcohol consumption immediately. Your doctor can help you develop a treatment plan if you need assistance.
• Other Triggers: Some people have observed that allergies, certain foods or environmental factors trigger their symptoms. You can gain insights by tracking them over time. For this, keep records of your symptoms and flare-ups to help you anticipate and treat the symptoms and update the specialist during your next dermatologist consultation.
Treatment for Psoriasis
Psoriasis treatments include creams, ointments (topical therapy), and medication plans aimed to stop skin cells from growing out quickly. Other options entail light therapy (phototherapy) and oral or injected medications. Your treatment plan depends on the severity of the disease and how responsive it has been to previous therapies. Self-care measures are also very effective. During a dermatologist consultation, your specialist will often advise patients to try different medications or treatments to find an approach that works. Even with successful treatment, the disease usually returns.• Topical therapy: During your dermatologist consultation, you will be prescribed applicative drugs for mild to moderate psoriasis. The medications are available in various forms like oils & ointments, creams, gels, foams, sprays and even shampoos. Specific medicines are applied during flare-up periods and alternate days or weekends during remission. Your specialist can prescribe stronger creams or ointments for smaller, less-sensitive, tougher-to-treat areas. However, long-term use or overuse of meds like potent corticosteroids can thin the skin. Also, over time, topical corticosteroids may stop working.
• Light Treatment: The therapy involves exposing the affected area to controlled intensity of natural or artificial light. Light treatment is advised for moderate to severe psoriasis or coupled with medications. Repeated treatments are necessary.
• Oral /injected meds: Your specialist may prescribe oral or injected drugs for psoriasis if other treatments have failed. Some of these medications are used for brief periods and are alternated with other therapies as they have the potential for severe side effects.
• Steroids: For certain types of symptoms, your specialist can suggest an injection. Other medicines reduce the production of skin cells, disrupt the flare cycle, and improve symptoms and signs of disease within weeks. Your skin expert, at your next dermatologist consultation, may prescribe specific oral medication to suppress the immune system. But patients cannot use certain meds to treat psoriasis for extended periods as many immunosuppressant drugs can increase the risk of infection or other health problems, including cancer.
• Alternative medicine: Studies claim that alternative therapies can also help ease the symptoms of psoriasis. Examples of alternative treatments used by people with psoriasis include acupuncture and herbal products applied to the skin. Although there is not much research to confirm their efficacy, they are safe and help ease itching and scaling for some people with mild to moderate psoriasis.
a. Aloe extract cream/ gel: The cream or gel is extracted from the aloe vera leaves and applied on the affected areas to reduce scaling, itching and inflammation. You will need to use the cream throughout the day for a month to notice improvements in your skin.
Home Remedies for Psoriasis
Try these self-care measures to manage psoriasis better:• Skin care during bath: Wash your skin gently while bathing. Bath in lukewarm water and use mild or herbal soaps with natural ingredients. You can add bath oils, Epsom salts or coconut milk to the bathwater and soak briefly before the bath.
• Keep skin moisturised: Apply moisturiser daily. If you're moisturising after the bath, gently pat yourself dry and apply your preferred product while the skin is still moist. Dry skin is itchy, and it can worsen the itch of psoriasis. Apply moisturiser daily. Use gentle soaps that won't dry out your skin. If the air is arid, use a humidifier to add moisture to the atmosphere. For dry skin, oils or heavy ointment-based moisturisers may be preferable as they stay on the skin longer than gels or lotions. If moisturising improves your skin, apply the product more than once daily.
• Get sunlight: Take regular walks in the morning to catch the sunlight. Early morning sunlight during walks can improve psoriasis. But for some people, intense sunlight, like sun tanning on the beach in the afternoon, can trigger or worsen psoriasis flare-ups and increase the risk of skin cancer.
• Ways to avoid scratching: a. Regular Application: Apply a non-prescription anti-itch cream or ointment recommended by the specialist at your dermatologist consultation. b. Medicated products: Try a medicated shampoo to treat psoriasis issues on the scalp. c. Trim nails: Keep your nails trimmed so they won't hurt your skin if you scratch. d. Clothing: Wear soft fabrics like cotton that do not irritate the skin.
• Avoid triggers: Observe what triggers the psoriasis symptoms and take steps to prevent or avoid it. Infections, injuries to your skin, tight clothes or intense humidity can worsen psoriasis.
• Stay cool: Higher than-normal temperatures can irritate the skin and aggravate psoriasis. Wear light cotton clothing if you're outside on hot days. Tight synthetic clothes can trigger the condition. Use air conditioning on hot days to keep cool. Also, keep cold packs in your freezer and apply them on itchy spots for relief. You could store your moisturising lotion in the refrigerator for a cooling effect.
• Healthy lifestyle: Try practising self-care and other healthy habits to manage psoriasis. Self-care includes: a. Exercising regularly. b. Eating nutritious and balanced meals. c. Limiting or avoiding alcohol consumption. d. Maintaining a healthy weight.
• Reduce stress: Stress triggers psoriasis. Cut down on stress in your life. Make time for what is essential for you and turn down additional responsibilities. Find ways to cope with the stress you feel, such as doing things you enjoy. Include activities like meditation, yoga, and spending time with friends, family and loved ones.
Foods to Avoid during psoriasis
Many high-calorie foods can cause weight gain & obesity, diabetes and heart disease can also be inflammatory. The following categories of inflammatory foods can worsen psoriasis symptoms:• Alcohol: Excessive alcohol consumption overburdens your liver. The liver has to produce chemicals to metabolise the alcohol, which can lead to inflammation in the long run if you drink heavily or regularly. Alcohol can also damage good gut bacteria, leading to inflammation in your colon and intestines and worsening psoriasis.
• Dairy: Many dairy products are high in fat, leading to inflammation. Cow milk products also contain casein, a protein that can be indigestible, and those who are lactose intolerant do not have enough lactase, a digestive enzyme. Also, gastrointestinal irritation from such conditions can worsen inflammation. Studies have shown that psoriasis symptoms improve when patients cut dairy from their diet.
• Refined carbohydrates: Refined carbohydrates like white bread, white rice, pasta, pastries and some breakfast cereals have been stripped of fibre and whole grains and contain sugar, which can cause your blood sugar to spike and lead to a psoriasis outbreak.
• Saturated fats and transfats: Studies have established that red meat, cheese, fried food, margarine, and processed snacks are loaded with fats that trigger inflammation in the body. Also, fats increase the amount of low-density lipoprotein (LDL) in the blood, called 'bad cholesterol. Studies have also shown a link between excess body fat, psoriasis development, and worsening psoriasis symptoms.
• Sugar: The synthetic sugars in soda, fruit juices, candy, baked goods, sweets, and other processed foods differ from natural sugars in natural food such as fruits. The pancreas produces the hormone insulin to process sugar, but excessive sugar compels our system to store that extra energy in fat cells that inflames the fat tissue. Foods with added sugars can also increase inflammatory protein levels called cytokines. Studies suggest that artificial sweeteners may also lead to chronic inflammation.
Foods to Eat During Psoriasis
Eat foods that help boost immunity and beat inflammation. Remember that psoriasis is an inflammatory condition. Although research is limited, many psoriasis patients have observed that they can manage the symptoms better if they eat more inflammation-fighting foods. It is essential to remember that just as some foods trigger inflammation, others can help combat inflammation throughout the body. Have a balanced whole-food diet, as healthy foods can reduce psoriasis flare-ups or make your symptoms less severe. Also, the best way to get all the nutrition, vitamins, and minerals you need is from the foods you eat regularly.The best foods to help beat the psoriasis symptoms include: • Tofu or tempeh • Fruits & vegetables • Legumes (beans & lentils) • Nuts & seeds • Whole grains
Living with Psoriasis
Psoriasis is a lifestyle disease, and patients are at higher risk for related conditions, like cardiovascular disease, depression and type 2 diabetes. The associated diseases are known as co-morbidities. It can have a detrimental effect on a person's quality of life.• Stigma: Many research studies have shown that psoriasis carries a high level of stigma. Many of the study participants believed psoriasis was infectious and contagious. Psoriasis is neither infectious nor contagious. The disease may make you feel isolated. Patients often think no one understands them, but they are not alone. Many people who have psoriasis are going through the same concerns, and they are thriving.
• Public spaces: The first step is to learn how to handle psoriasis at your workplace and teach your children to manage it at school if they suffer from the symptoms. Managing the disease includes speaking about psoriasis to teachers, your children's friends' parents, other students, managers and co-workers. There are many ways to help people understand your situation and what you are experiencing.
• Relationships: It may be difficult to confide in your partner, friends and family about psoriasis and how it affects your life initially. You'll probably feel self-conscious or think the symptoms may drive people away. Embarrassment is natural, and the people who care about you want to know how to support you. Doctors counsel patients to have these conversations and embrace them.
• Wear a psoriasis-friendly wardrobe: Although specialists encourage patients to have an open discussion with their family and immediate circles, patients are embarrassed about their skin condition. You may not want it to be the first thing someone sees. Certain clothes and fabrics, combined with moisturising, can enable you to look your best and feel your best in any situation or season. When you have psoriasis, your workout clothes can significantly affect how much you enjoy being active. Tight spandex and sweat may irritate your skin, so plan on wearing loose, breathable clothing. Cotton is a great choice, along with fabrics such as rayon and modal. Choose clothing that helps you feel comfortable and confident.
• Organising medical information: Keep an up-to-date file with your medical history, a record of the psoriasis outbreaks and their frequency, allergies, and medications, along with your insurance contact information. The details will help you recall and be easier to refer to during your dermatologist consultation.
• New routines: Start a new routine to stay focused on a positive future. Start slowly. Focus on a balanced lifestyle along with a healthier meal plan and ease into exercises at a steady pace. Don't dive into vigorous exercise if your body isn't used to it. For example, you can set aside time to take regular walks around your neighbourhood and aim to build up your fitness level over time. Also, update your specialist when changing your exercise routine during your next dermatologist consultation. If you're worried about aggravating your psoriasis condition or becoming injured, the skin specialist can suggest safe ways to get active.