What is Ringworm?
Ringworm (also called tinea or dermatophytosis) is a common fungal skin and nail infection that has no connection with worms. Ringworm is so named because it causes a red, itchy, circular (ring-shaped) rash. It can occur nearly anywhere in the body and is known by various names based on the body part it usually affects.Ringworm fungi thrive in warm, moist environments. This disease is highly contagious and spreads through direct contact with infected persons, animals, or contaminated surfaces. Ringworm can affect people of all ages. However, some groups may be more vulnerable to contracting Ringworm. Children are at a higher risk of developing Ringworm disease. Given its contagious nature and common occurrence, it is crucial to understand the symptoms of Ringworm disease, its causes, and the possible treatment.
Types of Ringworm
Ringworm can affect various parts of the body. It is classified according to its location. The types of Ringworm are as follows:- Tinea Corporis
- Tinea Capitis
- Tinea Pedis
- Tinea Unguium
- Tinea Barbae
- Tinea Faciei
Each type of ringworm disease requires care and appropriate treatment to prevent its spread. If you are concerned about having Ringworm, book an appointment with a trusted doctor and seek medical treatment as soon as possible.
Symptoms of Ringworm Disease
Ringworm symptoms on the body typically appear 4–14 days post-exposure to the fungus. Ringworm can appear anywhere on the body, including the fingernails and toenails.Typical symptoms include:
- a ring-shaped rash
- red, scaly, or cracked skin
- hair loss
- itchy skin
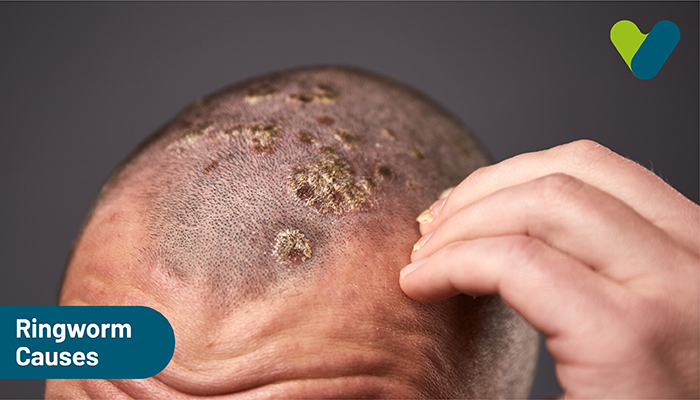
- Scalp ringworm appears as patches of hair loss and an itchy, scaly scalp with painful swelling.
- Athlete’s foot appears as itchy, cracked skin between the toes.
- Jock itch appears as a red, itchy rash in the groin area, sometimes extending to the inner thighs and buttocks.
- Nail ringworm causes the fingernails or toenails to become thick, discolored, and brittle.
Causes of Ringworm Disease
Over 40 different fungi can cause ringworm. These fungi are referred to as dermatophytes. Epidermophyton, Trichophyton, and Microsporum are specific dermatophytes linked to other types of Ringworm, including tinea capitis (scalp Ringworm infection), athlete’s foot, and jock itch. As specified above, Ringworm is caused by dermatophytes, a type of fungus. This fungus thrives on keratin, a protein that is found in the- nails,
- hair, and
- outer layer of skin.
Dermatophytes are microscopic spores that can live on the skin’s surface for months. They are adamant and can survive in the soil and on towels, combs, and other household items.
Dermatophyte spores can be transmitted from:
- Human to human Ringworm is frequently spread through direct skin-to-skin contact with someone who is infected.
- Animal to human Ringworm can be contracted by touching an infected animal. While grooming cats, dogs or during petting, ringworm can spread. It is also quite common in cows.
- Object to human Ringworm can be transmitted via contact with an item or a surface rubbed against or touched by an infected individual or animal, including garments, bedding, linens, brushes, and combs.
- Soil to human Rarely, ringworm can be transmitted to humans through exposure to the infected soil. Only prolonged contact with heavily infected soil would most likely result in infection. Children are especially vulnerable to ringworm infection. People who are born with a compromised immune system or who have had their immune systems compromised due to diseases like HIV/AIDS or certain medicines, such as chemotherapy drugs or corticosteroids, are at a high risk of developing this fungal infection.
Risk factors associated with ringworm
Ringworm can affect anyone, but one may be more susceptible if they:-
- Reside in a warm and humid climate or environment,
- Use communal locker rooms or showers,
- Take part in contact sports such as wrestling or football,
- Come into direct contact with animals,
- Have diabetes,
- Suffer from obesity or are overweight,
- Wear tight shoes or clothing that chafes the skin,
- Excessively sweat.
When to see a doctor?
You should consult a doctor when you have concerns about ringworm disease. Ringworm is a highly contagious disease, so early detection can make treatment more effective.If the symptoms of ringworm are not subsiding after two weeks of treatment, it could mean the infection is severe, requiring a more potent medication. You should see the doctor if:
- You have been in contact with an infected person.
- There is little to no improvement after treatment begins.
- The ringworm rash has spread to other body parts, especially if treatment has already started.
- You have a weak immune system.
- You are unsure about your diagnosis.
Diagnosis of Ringworm
A doctor can usually diagnose the ringworm disease after examining the area affected and asking the individual about their symptoms and medical history. They may collect a small skin scraping and assess it under a microscope or send it to a laboratory to look for fungal characteristics. If symptoms do not improve within 2 weeks of treatment, the doctor may perform a biopsy (remove a small piece of affected skin) and send it to a lab for analysis.How common is Ringworm?
Ringworm is a common fungal infection. A significant percentage of the population suffers from ringworm at least once in their life. The World Health Organization classifies Ringworm as highly contagious. It spreads through direct skin-to-skin contact with an infected person or animal. It also spreads through shared objects like bedsheets. Ringworm disease is infectious before the symptoms emerge.
Complications of Ringworm
If Ringworm is left untreated, it can spread to other areas of the body and another person. Other complications of Ringworm include:- Hair loss and scarring
- Secondary infection occurs if bacteria enter broken skin
- Dark marks left behind at the site of infection
- Nail deformities
- Majocchi Granuloma is a rare infection that occurs when the fungal infection reaches the deeper layers of the skin.
Treatment for ringworm
To treat ringworm, the doctor can prescribe medications as well as recommend lifestyle changes. Medications Based on the severity of the ringworm infection, the doctor may prescribe different medications. Jock itch, athlete's foot, and body ringworm are all typically treated topically using antifungals such as:- Ointments
- Creams
- Sprays
- Gels
- Disinfecting the surroundings and washing the bedding and clothing on a daily basis
- Drying the skin thoroughly after bathing
- Wearing loose clothing in affected areas
- Treating all the affected regions, as not treating them can result in a recurrence of the infection.
Prevention for ringworm
If ringworm occurs in a household, the following strategies may help prevent its spread:- A veterinarian should be consulted if a pet is the cause of the infection.Everyone must regularly wash their hands with soap.
- Hairbrushes, combs, clothing, bed linen, towels, and footwear should not be shared.
- Hot water and antifungal soap should be used to wash clothes.
- Anyone suffering from ringworm should avoid scratching affected areas, because this
- increases the likelihood of the infection spreading.
- Wearing loose clothing and staying cool may aid in lowering the risk.
- People should avoid walking barefoot in the house.
Home remedies for Ringworm
If you have contracted Ringworm disease, the aim is to prevent its spread. Prescribed and over-the-counter medications are the best methods to tackle the matter at the root.However, home remedies can help you manage the symptoms while recovering. These are the following ways you can treat Ringworm at home:
- Antibacterial soap and water keep the area clean. Wipe off excess water after washing and let it dry completely before applying medication or another home remedy. Moisture will help the fungus spread, so ensure it is completely dry.
- Apple cider vinegar has antifungal properties; soak a cotton ball with apple cider vinegar and brush it over the infected area.
- Tea tree oil and coconut oil have antifungal properties. You can apply both types of oil directly to the affected area two to three times per day with a cotton ball or swab. This remedy works best for scalp ringworm as coconut oil is a natural hair conditioner.
- Turmeric and aloe vera have antibacterial properties that help treat fungal infections by relieving some of the discomfort, like itching or burning.